In 2026, doctors are seeing something worrying. Adults under 50 with high visceral fat have up to three times higher risk of heart disease, according to recent data from the American Heart Association. The problem? You can’t see visceral fat the way you see loose or “jiggly” belly fat in the mirror. It hides deep inside the abdomen, silently affecting your organs. Most people think belly fat is just one thing. It’s not. There are two main types. Subcutaneous fat sits under the skin. It acts like padding and, in moderate amounts, is relatively harmless. Visceral fat is different. It wraps around organs like the liver, pancreas, and intestines. More importantly, it behaves like an active gland. It releases inflammatory chemicals, disrupts hormones, and interferes with insulin function.
This guide breaks it down clearly — what visceral fat really is, how it differs from subcutaneous fat, why it’s more dangerous in 2026 than ever, what causes it, how to measure it properly, how to reduce it in a practical way, common myths, and how to prevent it long term. Let’s start with the basics — because when it comes to metabolic health, your waistline often matters more than the number on the scale.
Defining Visceral and Subcutaneous Fat
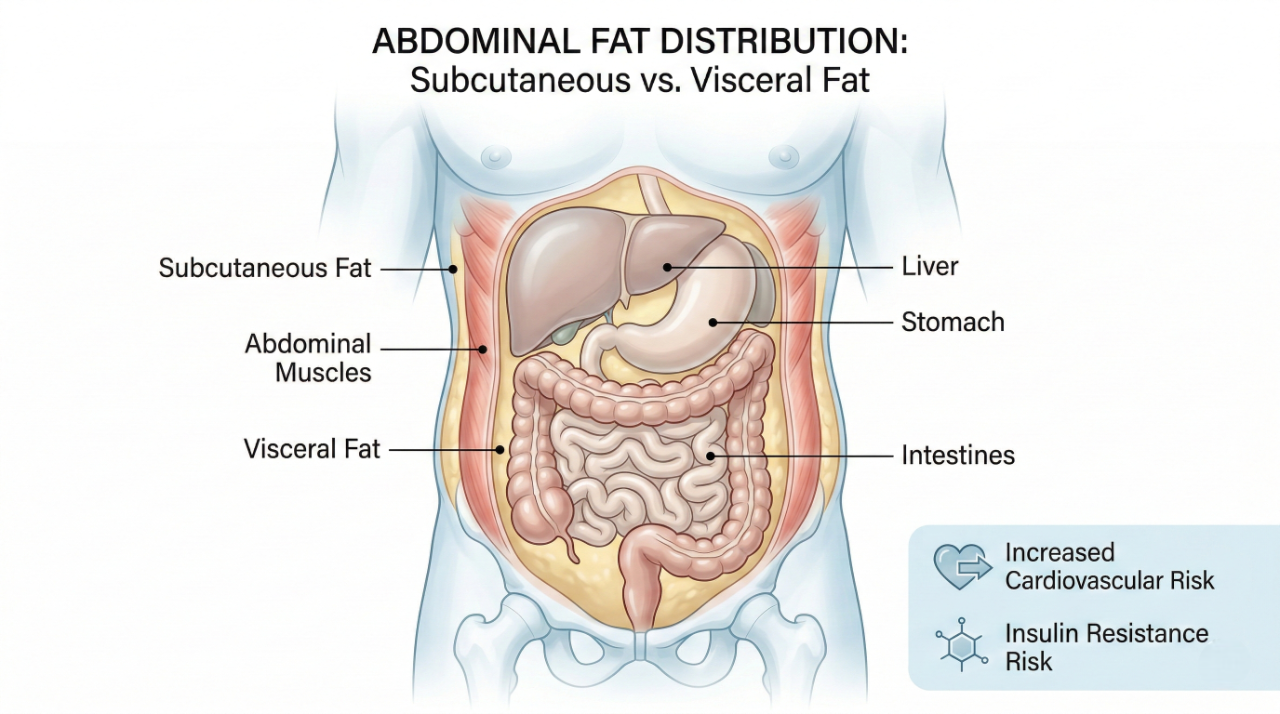
Belly fat is not just one layer. It is divided into two main types — visceral fat and subcutaneous fat — and they behave very differently inside the body.
Visceral fat sits deep inside the abdomen. It wraps around organs like the liver, pancreas, and intestines. You cannot pinch it with your fingers. It feels firm because it is packed tightly between organs. In healthy individuals, visceral fat usually makes up about 6–20% of total body fat. The problem is not just where it sits, but how it behaves. Visceral fat is metabolically active. It releases fatty acids and inflammatory chemicals directly into the bloodstream, especially toward the liver, which can disturb blood sugar, cholesterol, and hormone balance.
Subcutaneous fat, on the other hand, sits just under the skin. This is the soft fat you can pinch around your belly, hips, or thighs. It acts as an energy reserve and provides insulation and cushioning. In moderate amounts, it plays a protective role and does not directly harm organs. In 2026, technology has made fat estimation easier. Some AI-based body scanning apps, including tools developed around companies like Bodyspec, now use smartphone images and algorithms to estimate body fat distribution. While not as accurate as medical imaging, they are increasing awareness.
Key Differences Between Visceral and Subcutaneous Fat
| Aspect | Visceral Fat | Subcutaneous Fat |
| Location | Deep inside the abdomen, around the organs | Under the skin |
| Texture | Firm, tightly packed | Soft, jiggly |
| Health Impact | High metabolic and heart risk | Lower direct risk |
| Gender Bias | More common in men and post-menopausal women | More common in women, especially lower body |
Analysis: The biggest difference is location. Visceral fat sits close to vital organs and drains into the portal vein, which carries blood directly to the liver. This direct access to the bloodstream allows it to influence cholesterol, blood sugar, and inflammation quickly. Subcutaneous fat does not have this same metabolic impact.
Why Visceral Belly Fat Is Dangerous?
Visceral fat is dangerous because of how it interacts with your organs. It does not just sit there. It releases fatty acids and inflammatory chemicals called cytokines. These substances travel directly to the liver through the portal vein. Over time, this constant flow overloads the liver. When the liver is exposed to excess fatty acids, it becomes less responsive to insulin. This leads to insulin resistance — the starting point of Type 2 diabetes. Blood sugar rises, insulin levels increase, and the body slowly moves toward metabolic dysfunction. The same process affects heart health.
Visceral fat increases LDL (bad cholesterol), triglycerides, and blood pressure. This significantly raises the risk of Heart disease and Stroke. The liver also suffers. Excess visceral fat contributes to Metabolic dysfunction-associated steatotic liver disease, previously known as NAFLD. If untreated, it can progress to inflammation and scarring .
Research also links high visceral fat to Colon cancer, Breast cancer, and even Alzheimer’s disease, largely due to chronic inflammation and hormone disruption. In 2026, another concern has emerged. After the pandemic, doctors observed a rise in central obesity.
Data from the International Diabetes Federation shows roughly one in three adults globally now has a metabolic risk linked to excess abdominal fat. Post-COVID metabolic changes and reduced physical activity have contributed to this surge, and some long-haul symptoms are worsened by persistent inflammation. In contrast, subcutaneous fat is mostly harmless unless excessive. It can cause joint strain or cosmetic concerns, but it does not directly flood organs with inflammatory chemicals.
A practical example: people with an “apple-shaped” body — waist circumference above 40 inches in men — have nearly double the mortality risk compared to those with lower abdominal fat. Waist size often predicts risk better than total weight.
Causes of Visceral Fat Buildup
Visceral fat does not increase randomly. It builds up slowly due to a mix of diet, lifestyle, hormones, and genetics. Diet is the biggest driver. Regular intake of sugar, especially fructose (found in soft drinks, packaged juices, sweets), pushes the liver to convert excess sugar into fat. Processed carbohydrates like white bread, bakery items, and refined snacks spike insulin repeatedly. Over time, this promotes fat storage deep inside the abdomen rather than under the skin. Lifestyle matters just as much.
Long hours of sitting reduce fat burning. Stress raises cortisol, a hormone that encourages fat storage around the belly. Poor sleep — less than 6 hours regularly — disrupts hunger hormones and insulin sensitivity, increasing visceral fat even if calorie intake stays the same. Genetics also plays a role. Some people are naturally more prone to storing fat centrally. Alcohol adds another layer, as excess intake overloads the liver and promotes abdominal fat accumulation. Smoking, despite suppressing appetite in some cases, is linked with higher visceral fat distribution.
A clear 2026 trend is the remote work “skinny-fat” pattern. Many young professionals have a normal BMI but high visceral fat due to inactivity, stress, and irregular eating. They look average in weight but carry metabolic risk internally — a silent issue that often goes unnoticed until blood tests reveal problems.
How to Measure Visceral Fat?
You cannot see visceral fat directly, so measurement matters. The simplest method is waist circumference. For most populations, risk increases when waist size is above 94 cm (37 inches) in men and 80 cm (31.5 inches) in women. Measure at the level of your belly button, standing relaxed, not sucking your stomach in. Waist size often predicts metabolic risk better than body weight alone. In 2026, technology has improved access. DEXA scans can estimate visceral fat with good accuracy.
Some smart scales, like those from Withings, use bioelectrical impedance to give a visceral fat estimate. AI-based body scan apps also provide rough assessments, though they are not diagnostic. The gold standard remains CT or MRI scans, which directly visualize fat around organs. However, these are usually done only when medically necessary. Actionable tip: Measure your waist weekly under the same conditions. Tracking trends matters more than a single reading.
Proven Reduction Strategies for Visceral Fat
Reducing visceral fat is not about crash dieting. It needs a combined approach — food, movement, and daily habits working together. Spot reduction does not work. But consistent metabolic improvement does.
Exercise Matters Most
Visceral fat responds well to structured activity. Research consistently shows that exercise can reduce it even without dramatic weight loss.
| Method | Impact | Protocol |
| HIIT | 10–20% faster visceral reduction | 20 minutes, 3 times per week |
| Strength Training | Increases muscle, improves insulin sensitivity | Squats, lunges, push-ups, planks — 3 times per week |
| Cardio/Walking | Steady fat loss lowers inflammation | 8,000–10,000 steps daily |
HIIT improves insulin response quickly. Strength training builds muscle, which increases resting metabolism. Even daily brisk walking reduces liver fat over time.
Diet: Keep It Practical
The Mediterranean diet has strong evidence behind it. It focuses on vegetables, fruits, olive oil, nuts, fish, and whole grains. It reduces inflammation and improves lipid levels. Low-carb approaches also help by lowering insulin spikes. Many adults benefit from 16:8 intermittent fasting, where food is eaten within an 8-hour window. This improves insulin sensitivity and encourages the body to use stored fat. The key is reducing added sugar and ultra-processed food — especially liquid calories.
Habits That Protect Metabolism
Sleep 7–9 hours consistently. Poor sleep raises cortisol and increases belly fat storage. Manage stress. Chronic stress pushes fat toward the abdomen. Simple practices like yoga, breathing exercises, or regular outdoor walks lower cortisol levels.
What Results Look Like?
Clinical studies show that consistent lifestyle change can reduce visceral fat by around 14% within six months — even without extreme dieting. The focus should not be just weight loss. The real goal is lowering inflammation, improving insulin function, and shrinking harmful fat around organs.
Myths Busted
Myth 1: Spot reduction works.
Doing 200 crunches daily will not selectively burn belly fat. Fat loss happens systemically. The good news? Visceral fat is often the first to reduce when you improve your diet and exercise consistently.
Myth 2: Beer alone causes a beer belly.
It’s not just beer. It’s excess calories overall — from alcohol, fried snacks, sugary mixers, and late-night eating. Alcohol does worsen fat storage around the liver, but total energy balance matters more.
Myth 3: You must follow keto forever.
Extreme diets may show quick results, but the 2026 metabolic guidelines focus on sustainability. Whether it’s moderate carbs, Mediterranean, or time-restricted eating, long-term adherence matters more than short-term restriction.
Conclusion
Visceral fat is far more dangerous than subcutaneous fat because it directly affects organs, hormones, and inflammation. It increases the risk of diabetes, heart disease, fatty liver, and even cognitive decline.The first step is simple: measure your waist. If it is rising, act early. Add structured movement like HIIT or strength training. Improve food quality. Sleep better. Long-term prevention is not about perfection. It is about consistent habits. With better awareness, smarter tracking tools, and clear research in 2026, reducing belly fat is no longer confusing. It is practical — if you take action now.


